Cognitive behavioural therapy (CBT) and dialectical behaviour therapy (DBT) are both widely used in psychotherapy.
CBT, often heralded for its structured approach, aims to alter negative thought patterns and behaviours to mitigate distress and develop healthier coping mechanisms. It operates on the premise that altering one’s thought processes can significantly impact feelings and behaviours, leading to improved mental health outcomes.
Conversely, DBT extends the foundational principles of CBT to specifically cater to people experiencing heightened emotional distress, offering a lifeline to those struggling with intense emotional reactions or self-destructive behaviours. It introduces the concept of mindfulness and emotional regulation as core components, guiding individuals through the tumultuous waters of their emotions and promoting a balance between acceptance and change.
History of CBT and DBT
Aaron T. Beck’s pioneering work in the 1960s laid the groundwork for CBT by linking the impact of thoughts on emotions and behaviours, introducing a goal-oriented therapy to counteract negative thinking patterns. This approach gained prominence for its applicability across various mental health conditions, championing the idea that changing maladaptive thoughts could lead to significant emotional and behavioural improvements.
Marsha M. Linehan’s creation of DBT in the late 1980s addressed a gap in treatment for people with borderline personality disorder who experienced deep emotional instability and engaged in self-destructive actions. DBT expanded on CBT’s principles, incorporating mindfulness and distress tolerance to equip patients with tools for navigating intense emotions and improving interpersonal relationships.
Both therapies have undergone considerable refinement and are endorsed by a substantial body of research, demonstrating their efficacy in treating a wide array of psychological disorders. They represent key milestones in psychotherapeutic treatment, embodying a shift towards more empathetic, client-centred care that acknowledges the complexity of human emotions and behaviours.
Core Principles of Each Therapy
Cognitive behavioural therapy and dialectical behaviour therapy share common ground in their dedication to improving mental health, yet each unfolds through distinct core principles. CBT centres on the interconnection between thoughts, emotions, and behaviours. It emphasises identifying and modifying negative thought patterns and behaviours to enhance emotional well-being. This therapy equips people with strategies to challenge and alter detrimental thoughts, aiming for a shift towards more positive and constructive thinking.
DBT, while encompassing the essence of CBT, places a greater emphasis on emotional regulation and mindfulness. It introduces the concept of dialectics, advocating for the acceptance of conflicting thoughts, feelings, and behaviours as a pathway to change. DBT’s core principles also include distress tolerance and interpersonal effectiveness, focusing on teaching people how to live in the moment, cope with stress in healthy ways, manage intense emotions, and improve relationships.
Both therapies highlight the importance of developing coping mechanisms that effectively manage challenging thoughts and feelings, underscoring their complementary roles in the therapeutic landscape.
Therapeutic Goals and Strategies
Exploring the therapeutic goals and strategies of CBT and DBT demonstrates their nuanced approaches to improving mental health.
Cognitive Behavioural Therapy
CBT is designed to modify detrimental thought patterns and behaviours that contribute to a person’s distress. Its goals are multifaceted, including cognitive restructuring to challenge and alter negative thought patterns, behavioural modification to develop healthier coping mechanisms, and the reduction of symptoms related to mental health conditions such as anxiety and depression.
The strategies used in CBT, like homework assignments, role-playing, and systematic desensitisation, are aimed at applying learned techniques in real-world settings, preparing individuals for challenging interactions, and reducing fear or distress related to specific triggers.
Dialectical Behaviour Therapy
Conversely, DBT’s objectives are rooted in balancing acceptance of one’s current life situation with the drive to enact change, enhancing emotional regulation to manage intense emotions effectively, and improving interpersonal relationships and distress tolerance.
The strategies employed in DBT encompass mindfulness exercises to promote living in the moment, distress tolerance skills to cope with immediate stress, and interpersonal effectiveness training to better navigate conflict and communicate more effectively.
Both CBT and DBT offer comprehensive frameworks for therapy, but their goals and strategies reflect their tailored approaches to addressing mental health issues.
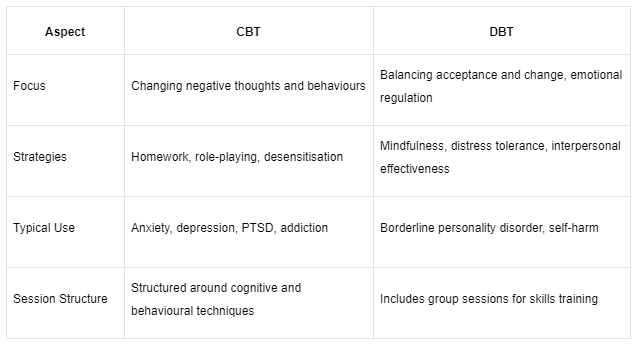
Who Is Each Modality For?
Cognitive behavioural therapy is typically recommended for people experiencing:
- Depression
- Addiction
- Anxiety
- Phobias
- Other stress-related conditions
It works well for those seeking to address negative thought patterns and behaviours that impact their daily functioning and mental well-being. CBT is particularly effective for conditions where altering thought processes can significantly improve how a person feels and acts.
Dialectical behaviour therapy, on the other hand, is suited for people dealing with more intense emotional disturbances. It’s particularly beneficial for those diagnosed with borderline personality disorder, engaging in self-harm, or having chronic suicidal thoughts. DBT helps people who experience overwhelming emotions, offering them strategies to manage these feelings more effectively and build better relationships.
Both CBT and DBT offer valuable tools for addressing mental health challenges, with the choice between them depending on the nature and severity of the conditions faced. Engaging with a mental health professional can help determine the most appropriate therapy based on specific needs and therapeutic goals.
Comparison of Techniques and Sessions
Cognitive behavioural therapy sessions usually last about 50 to 60 minutes and can be conducted 1:1 between therapist and client. The duration of treatment varies, often spanning 5 to 20 sessions, depending on the specific needs and the progress being made.
Dialectical behaviour therapy, in contrast, includes both 1:1 therapy and group skills training sessions. Individual sessions, which last approximately the same duration as CBT sessions, examine personal challenges and use DBT strategies to manage emotions and improve relationship skills.
However, DBT is distinct in that it incorporates weekly group sessions that focus on teaching and practising core principles. These group sessions are an essential component of DBT, providing a supportive environment for learning and applying skills. A comprehensive DBT programme typically extends over 6 to 12 months.
The choice between CBT and DBT depends on the client’s specific conditions and therapeutic goals, with both modalities offering unique approaches to enhancing mental health through structured therapeutic techniques.
Effectiveness and Outcomes
Research shows that both types of therapy are effective across various conditions, demonstrating significant improvements in mental health outcomes.
CBT has been shown to be effective for social anxiety disorder, panic disorder, obsessive-compulsive disorder, and post-traumatic stress disorder. It’s also got a proven track record of helping people with addiction, with one study finding that 60% of people who received CBT provided clean toxicology samples one year later.
A study on people with BPD found that after receiving DBT treatment for one year, 77% no longer met the criteria to be diagnosed with the condition, and meta-analysis of various studies showed that DBT significantly reduced suicidal ideation, self-injurious behaviour and frequency of crisis psychiatric service visits by a large degree.
Find Out How Therapy Can Help You
Exploring the landscapes of cognitive behavioural therapy and dialectical behaviour therapy reveals their profound capacity to transform lives. Whether you’re dealing with depression, anxiety, or more complex emotional challenges, these therapies provide a pathway to recovery.
Ishmail & Associates offers both CBT and DBT as part of our comprehensive mental health service, and our dedicated team is committed to supporting your journey towards well-being.
If you or a loved one is navigating mental health challenges, we invite you to consult with our professionals to determine the most fitting support for your situation. Together, we can embark on a recovery path tailored to your specific needs.
Sources:
- https://guilfordjournals.com/doi/abs/10.1521/pdps.2015.43.3.423
- https://psychotherapy.psychiatryonline.org/doi/abs/10.1176/appi.psychotherapy.2015.69.2.97
- https://psycnet.apa.org/journals/bct/9/2/1/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3584580/
- https://pubmed.ncbi.nlm.nih.gov/18363421/
- https://pubmed.ncbi.nlm.nih.gov/17636720/
- https://pubmed.ncbi.nlm.nih.gov/15533282/
- https://pubmed.ncbi.nlm.nih.gov/12215081/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4579507/
- https://www.sciencedirect.com/science/article/abs/pii/S0005789418300492
- https://www.sciencedirect.com/science/article/abs/pii/S0005789418300492
